Urology beyond Europe: Different approaches, same goal
The mission of the European Association of Urology (EAU) is to raise the level of urological care throughout Europe and beyond. A central pillar of this mission is the exchange of high-quality urological information with other societies around the world. That is why the first day of EAU21 Virtual featured 16 “Urology beyond Europe” sessions, each organised in collaboration with a different society and each focussing on a variety of urological topics from a unique geographical point of view.
PSA screening in Europe and South Korea
A case in point of an international exchange of advice and information was the Joint Session of the EAU and the Korean Urological Association. One of the topics addressed was PSA screening for prostate cancer (PCa). Dr. Giorgio Gandaglia (IT) introduced his lecture as “the European perspective on structured population-based screening for PCa.” He said, “The use of baseline PSA levels, risk calculators, multiparametric MRI, and biomarkers can improve the effectiveness of a PSA screening approach, reducing the risk of overdiagnosis and overtreatment” (see figure 1). Answering critical questions asked by Prof. Philip Cornford (GB), Dr. Gandaglia indicated that a combination between tailored and mass screening is best, as his slide showed.
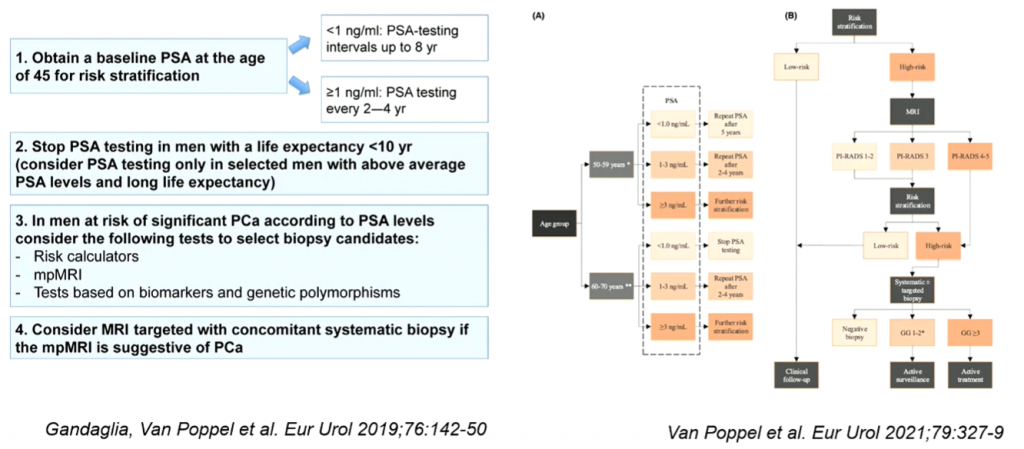
Figure 1. You can find a more legible version of the scheme on the right in the original article.
In South Korea, the National Cancer Screening Program does not include PCa screening. Prof. Jae Young Park (KR) asked Dr. Gandaglia whether there are any protocols for PSA screening in effect in Europe and whether there are any differences among European countries. Dr. Gandaglia answered that there are, indeed, differences among European countries as for how to approach PSA screening. The EAU is pushing for a universal European approach.
Dr. Gandaglia ended the session as panellist together with Prof. Park, both giving advice about a clinical case involving oligometastatic PCa presented by Prof. Seung Hwan Lee (KR).
Transection versus non-transection of the bulbar urethra
The Société Internationale d’Urologie and the EAU share the same mission, and their joint session involved a wide variety of hot topics focussed on improving the patient care, mainly surgical in nature. For example, the first of the two debates dealt with the transection-vs-non-transection-of-the-bulbar-urethra question. Prof. Anthony Mundy (GB) summarised his lecture with saying that, “The non-transecting approach to bulbar urethroplasty for idiopathic strictures gives the freedom to choose the best technique for each patient according to the nature of the stricture and to minimise surgical trauma without compromising effectiveness. Nowadays in our practice, the only indication for transecting bulbar urethroplasty is for traumatic strictures.”
Dr. Allen Morey (US) gave his lecture the fitting name “Pro: Anastomotic Urethroplasty (Transection)” and went on to say that “we believe [transection and anastomosis in bulbar urethral reconstruction] is still the gold standard today.” In his next slide, he gave three reasons for this (see figure 2). “Optimal exposure allows complete scar removal and optimal outcomes. The concerns on erectile dysfunction are poorly defined and lack a significant anatomic or physiologic basis. Furthermore, the wide applicability for the transecting approach applies to patients that are typically seen at referral centres in whom the strictures can be quite challenging.”
In the ensuing debate, Dr. Mundy came to the conclusion that Dr. Morey was actually “furiously agreeing” with him, alluding to a tailored approach to each patient. “You do what is best for your patient.”
With that, this debate became a symbol of the Urology beyond Europe sessions: the approaches may differ, but everyone’s goal is the same.
Figure 2
On Thursday, the EAU held, in chronological order, joint sessions with the Russian Society of Urology, the Urological Society of Australia and New Zealand, the Federation of ASEAN Urological Associations, the Taiwan Urological Association, the Korean Urological Association, the Japanese Urological Association, the Pakistan Association of Urological Surgeons, the Iranian Urological Association, the Caucasus/Central Asian countries, the Société Internationale d’Urologie, the Urological Society of India, the Arab Association of Urology, the Maghreb Union countries, the Pan-African Urological Surgeons Association, the Confederación Americana de Urología, and the Canadian Urological Association. The recordings of all these sessions will become available in the “On Demand” feature on the EAU21 Virtual Platform.

